 At 1 year of follow-up, 77% were free of atrial tachycardia or atrial flutter and 61% were free of all atrial arrhythmias.įor decades, there was a scientific debate as to whether or not typical atrial flutter was focal or reentrant. Thus, 28/31 (90.3%) terminated with RF energy and/or could not be reinduced after ASC ablation. Median time from initial ablation to AAF termination was 64 s. AAF degenerated to atrial fibrillation in 2/31 (6.5%) with RF and could not be reinduced after ASC ablation. We targeted the ASC and ablation terminated AAF directly in 19/31 (61.3%) and altered AAF activation in 7/31 (22.6%), all of which terminated directly with additional mapping/ablation. Macroreentry atrial flutters took varied pathways, but each had an area of slow conduction (ASC) averaging 16 ± 6 mm (range 6–29) in length. 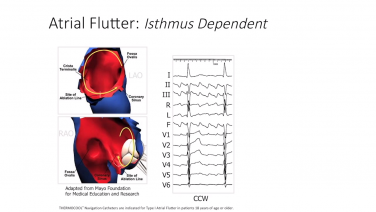
For every AAF, the entire circuit was identified. Time to create and interpret the UHD-ASM was 20 ± 11 min. For each AAF, 1273 ± 697 points were used for UHD-ASM. I have followed all appropriate research reporting guidelines and uploaded the relevant EQUATOR Network research reporting checklist(s) and other pertinent material as supplementary files, if applicable.Demographics age = 65.3 ± 8.5 years, male = 78%, left atrial size = 4.66 ± 0.64 cm, redo ablation 20/23(87%). I confirm that any such study reported in the manuscript has been registered and the trial registration ID is provided (note: if posting a prospective study registered retrospectively, please provide a statement in the trial ID field explaining why the study was not registered in advance). I understand that all clinical trials and any other prospective interventional studies must be registered with an ICMJE-approved registry, such as. 
Funding StatementĪll relevant ethical guidelines have been followed any necessary IRB and/or ethics committee approvals have been obtained and details of the IRB/oversight body are included in the manuscript.Īll necessary patient/participant consent has been obtained and the appropriate institutional forms have been archived. The authors have declared no competing interest. 
Further studies are needed to assess the usefulness of this tool for improving catheter ablation outcomes. Conclusion A low-density and prolonged LAT-Valley in a heterogeneous low-voltage area compose an electrophysiologic triad that allows the identification of the AFL critical isthmus. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
